Wake and Light Therapy for Depression & Sleep Deprivation
Wake and Light Therapy is a promising treatment for depression. Depression (in some individuals) is associated with disturbances in one’s circadian rhythm. The therapy can reset your rhythm to be back in sync with the sun and reset your internal clock.
Wake and Light Therapy
Wake and Light Therapy refers to a treatment that involves total sleep deprivation for 36 hours, followed by four days of advancing the time that you go to sleep. It also incorporates bright light therapy each morning.
Wake and Light Therapy is technically called Triple Chronotherapy. It is an emerging science, so it is unlikely to be included in the revised NICE Guidelines for treating depression. More research into Wake and Light Therapy is needed but I am excited about its potential. Our team have conducted a review of 4 previous trials and 12 case series in inpatients that was published in the Journal of Affective Disorders in 2020. Our conclusion was that chronotherapy appears to be effective for the rapid treatment of depression with about 50% of patients achieving recovery within the first week. We went on to conduct our own small controlled trial in out-patients and demonstrated similar results. This study was published in BJPsych Open in 2021.
The history of Wake and Light Therapy
Sleep deprivation was described in a German textbook of psychiatry in the 1880s. It did not develop until a German schoolteacher with depression reported to her psychiatrist that she could temporarily cure herself by a night-long cycle ride. We now know that it was not the exercise for one night that was required but it is an excellent way of staying awake.
The baton was picked up by Dr Burkhard Pflug in University of Tübingen, Germany who published his PhD on a case series of patients undergoing sleep deprivation in 1973. There were quite a few controlled studies on sleep deprivation in 1980-1990s. The problem was that in those people who respond in the first few days, there was a very high rate of relapse and most patients return to their previous state.
A couple of decades later, researchers found two ways of preventing the relapse with advancing the time patients go to bed each day for five days. The second involves using bright Light Therapy to help stabilise the response.
Why might the Wake and Light Therapy be of help?
A hormone, called melatonin, is released at night by the pineal gland in the brain to regulate both your sleep and other hormones. Some people release melatonin at the wrong time of the day. This is not the whole explanation as it’s likely to be more complicated.
The rationale for Wake and Light Therapy is that depression (in some individuals) is associated with disturbances in one’s circadian rhythm and the therapy can reset your rhythm to be back in sync with the sun. Thus, Wake Therapy is like Ctrl-Alt-Delete and resets your internal clock.
If we can reset this release to the right time of the evening, it can help control symptoms of depression. Another effect of sleep deprivation is a surge of mono-amines (for example serotonin, dopamine) and anti-inflammatory chemicals. Both are thought to be relevant in helping some types of depression.
Can the therapy be combined with standard treatments?
You can have the therapy with other treatments like Cognitive Behavioural Therapy and medication. You are more likely to get good results by combining these components with the therapy. The positive effects of Wake and Light Therapy can be enhanced by ensuring routine in your activity, sleep and eating. Patients often find this improves their mood and they have more energy to tackle other issues that can be contributing to their depression. Crucially, Wake Therapy can often then help patients focus on Cognitive Behaviour Therapy as well as effecting lifestyle changes and good sleep hygiene.
The practice of Wake and Light Therapy
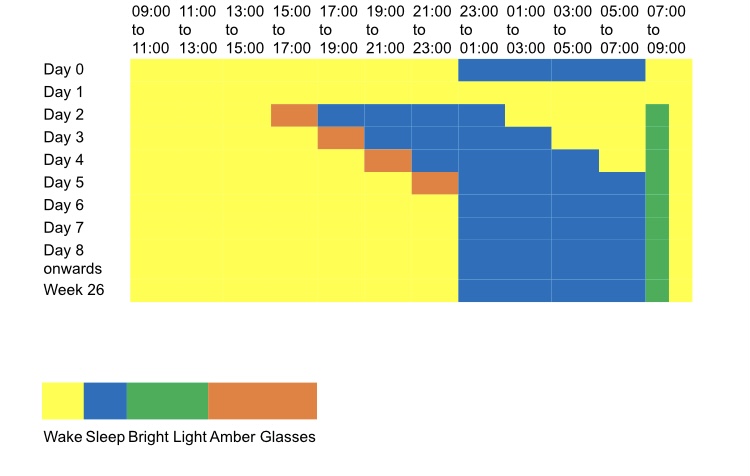
The following is a typical weekly Wake and Light Therapy treatment programme. You may read of variations in the timetable, but it’s not known yet if one approach is better than another. The most important thing is to stay fully awake during the periods of sleep deprivation. Napping will ruin what gains you might have made resetting your bodily clock.
Day 1 (Monday)
Note: you can start on any day of the week and some people find it’s best done starting on a Friday, so they go to work easily on the following Monday.
Before you begin, we assess the severity and type of your depression and the pattern of your sleep.
On the first night, you stay awake with no naps. On our ward, this is done with the support of a nurse and sometimes fellow patients in a small group. We plan activities for the night on the ward e.g., a short walk or an activity like cooking. Patients have access to coffee/tea and snacks.
Day 2 (Tuesday)
You may experience an immediate improvement in your mood but unless you continue with the program in the way we describe you are very likely to relapse.
You receive Bright Light Therapy (please see separate blog for detailed instructions) for 30 minutes sometime between 6.45am and 9am. The exact timing will depend on the results of our initial assessment but for most people is usually about 7am. You should sit about a foot (30cm) from the light with your eyes open. Ideally, the light screen should be tilted at a 15° angle toward you so that the light is projected over as you receive treatment. You should not stare at the light, but you may read, work, eat, etc. while receiving the light therapy. An alternative to Bright Light Therapy is to go outdoors first thing in the morning for natural sunlight especially in the Summer months.
You stay awake during the day and structure your activities as planned with your therapist. You should try not to have any naps. We encourage you to use amber glasses or lighting from 2pm as this provides virtual darkness and encourages the release of melatonin. This tells the brain that it is time to go to sleep in a few hours.
You then go to bed at 5pm and wake by 1am (i.e., about 8 hours sleep).
If you cannot resist a nap it should last no more than 10-15 mins before midday.
Day 3 (Wednesday)
You stay awake during the day, go to bed at 7pm and wake by 3am. After a light snack, the nursing staff on the ward provide some activity. Bright Light Therapy is provided for 30 minutes as described with the same timing as on Day 2.
We encourage the use of amber glasses or lighting from 4pm to prepare you for bed at 7pm.
There is a planned activity schedule and treatment as usual on the ward.
Day 4 (Thursday)
You stay awake during the day, go to bed at 9pm and wake by 5am. Again you receive Bright Light Therapy for 30 minutes at the same time as before.
We encourage the use of amber glasses from 6pm.
You have Bright Light Therapy at the same time as you did on Day 2 with similar activities and treatment on the ward.
Day 5 (Friday onwards)
By this point your sleep schedule should be getting back to normal. You go to bed by 11pm and wake by 7am. We encourage the use of amber glasses from 7pm.
Bright Light Therapy is provided for 30 minutes at the same time as on Day 2, and there are activities and treatment on the ward. In future you can carry on with the Bright Light Therapy in the morning but can discontinue with the amber glasses.
How will we know if there is any benefit?
Naturally, you will want to judge how effective the therapy is and whether there is a downside. One of the staff will rate your symptoms on a scale and we will ask you to complete some questionnaires at the beginning of the treatment and again at the start of the following week to assess progress.
David Veale
Scientific References
Wirz-Justice, A, Benedetti, F, Terman, M. (2012). Chronotherapeutics for Affective Disorders: A Clinician’s Manual for Light and Wake Therapy. Karger. Amazon
Humpston, C, Benedetti, F, Serfaty, M, Markham, S, Hodsoll, J, Young, AH & Veale, D (2020) Chronotherapy for the rapid treatment of depression: a meta-analysis. Journal of Affective Disorders, 261, 91-102.V
Veale, D., Serfaty, M., Humpston, C., Papageorgiou, A., Markham, S., Hodsoll, J., & Young, A. (2021). Out-patient triple chronotherapy for the rapid treatment and maintenance of response in depression: Feasibility and pilot randomised controlled trial. BJPsych Open, 7(6), E220. doi:10.1192/bjo.2021.1044